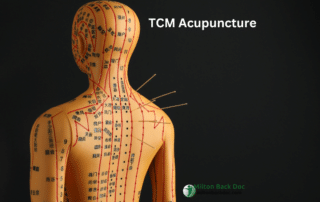
TCM Acupuncture At Milton Back Doc – Explore This Healing Artform
TCM Acupuncture At Milton Back Doc - Explore This Healing[...]
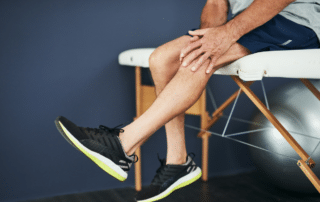
Knee Pain in Milton? Our Physiotherapy Team Can Help
Experiencing knee pain in Milton? You're not alone. Knee injuries[...]
Rotator Cuff Injury Recovery With Your Local Chiropractor
Rotator cuff injuries can be debilitating, affecting daily activities, athletic[...]
Preventing Concussion in Sport – Helmets
Patients looking for Concussion related treatment, baseline assessment[...]
Post Injury Assessment & Return-to-Activity
Concussions are a serious concern in sports and[...]
Baseline Testing: What to Expect & Benefits
In recent years, concussion awareness has risen dramatically,[...]